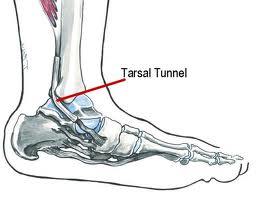
Tarsal Tunnel Syndrome
With tarsal tunnel syndrome, compression of the tibial nerve occurs within a tunnel created by a floor consisting of the calcaneus and bounded by the medial malleolus- the bump on the inside part of the ankle- and the far corner of the heel bone. The roof of the tarsal tunnel is formed by a retinaculum- a tough piece of fibrous tissue.
Within the tarsal tunnel run a number of tendons as well as the tibial nerve, and the posterior tibial artery.
In other patient, tarsal tunnel syndrome can occur even if the nerve compression is found elsewhere. A patient who has a pinched nerve in the low back along with tarsal tunnel syndrome. This condition, where there is compression at least two locations, is termed "double-crush" syndrome.
Another problem is that there are many people who have tarsal tunnel syndrome may have peripheral neuropathy. This is a condition where there is damage to the small nerves in the feet. A tingling sensation and numbness are typical symptoms. Among the diseases associated with peripheral neuropathy are diabetes and thyroid disorders.
Medications can also cause a peripheral neuropathy and various chemotherapy agents given for cancer.
Excessive alcohol and tobacco use as well can cause peripheral neuropathy as can exposure to heavy metals. The most common symptom of tarsal tunnel syndrome is foot pain, which can also be accompanied by numbness and tingling.
Tapping on the tibial nerve at the tarsal tunnel may cause pain and tingling to occur. The clinical impression can be confirmed with electrical testing (electromyography and nerve conduction). Electrical testing is important to evaluate the patient for other nerve entrapment problems such as a pinched nerve in the back. Peripheral neuropathy can also be diagnosed. Magnetic resonance imaging (MRI) and ultrasonography may be useful in evaluating a patient for underlying reasons for tarsal tunnel syndrome.
Medical therapy for tarsal tunnel syndrome may start with local injection of steroids into the tarsal tunnel. Physical therapy may be of some value in reducing soft-tissue edema which can ease pressure on the compartment.
Splints and braces may be helpful for patients who have anatomic abnormalities in the hindfoot and ankle.
When conservative therapy fails to help the patient's symptoms, surgical intervention may be warranted.
When a patient doesn't improve and has persistent pain, associated plantar fasciitis may be a cause of persistent pain in the medial heel region after surgery.
There is a plethora of advanced therapies, particularly MicroVas and TENS therapy. Both are instrumental in relieving symptoms, either as a preoperative modality or post operative, and therapeutic medicines such as as gabapentin are also helpful.
Call us now:
(239) 430-3668 (FOOT)
Self service # (239) 420-7170